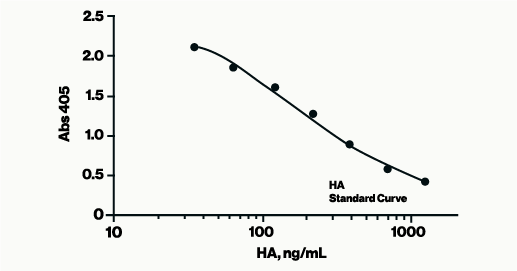
The Hyaluronan Enzyme-Linked Immunosorbent Assay (HA ELISA), a competitive 96-well assay, offers a simple, effective method for determining Hyaluronic Acid (HA) levels in human and animal biological fluids or cell supernatants.
Assay Range: 50-1600 ng/ml
Sensitivity: 25 ng/mL
Sample considerations: The HA ELISA detects HA molecules that are as small as 6.4 kDA.4
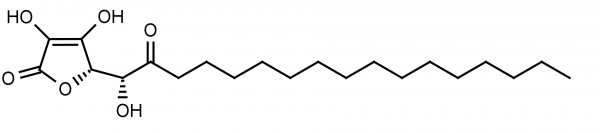
Hyaluronic acid (HA) is a high molecular weight anionic polysaccharide (1,000-10,000 kD) composed of repeating disaccharides. It is one of several glycosaminoglycan components of the extracellular matrix of connective tissue.
Free HA is taken up by the liver where it is degraded and recycled. Many chronic liver diseases, including infection (hepatitis B or C), toxicity (alcohol and drugs), genetic (hemochromatosis), autoimmunity, and malignancy, result in liver inflammation which can progress to liver fibrosis and cirrhosis; causing impairment of liver function and resulting in a rapid increase in circulating HA levels.
Data indicates a relationship between HA levels, local inflammation and severity of disease. Recent publications have shown HA levels in urine are indicative of bladder cancer, that HA levels are correlated to liver disease, and the breakdown of HA in the lungs of patients with chronic obstructive pulmonary disease. Additionally, serum levels of HA have been found to be elevated in patients with rheumatoid arthritis.
For help on selecting the correct HA detection assay see this Blog: Which Hyaluronic Acid Assay Should I Use? and this HA Assay Comparison Chart. orPowered by Bioz See more details on Bioz
For additional information on this product, see this Biocompare product review here.
Product Keywords: Hyaluronan, Hyaluronate, Liver Cirrhosis, Rheumatoid Arthritis, Hyaluronan, Osteoarthritis, Liver Fibrosis